Meniscus Transplant Study Group
A global collaboration of orthopaedic surgeons, veterinary surgeons, and scientists dedicated to advancing the science and clinical practice of meniscus transplantation.
About MTSG
What is a Meniscus?
The meniscus is a soft, fibrous cartilage structure that rests between the femur (thighbone) and tibia (shinbone) in the knee joint. Each knee contains two menisci: the medial meniscus on the inner side and the lateral meniscus on the outer side.
A healthy meniscus provides crucial cushioning and shock absorption, distributes forces evenly across the knee joint, and creates a gliding surface that is five times smoother than ice on ice. The meniscus plays a vital role in joint stability, lubrication, and protection of the articular cartilage.
What is Meniscus Allograft Transplantation (MAT)?
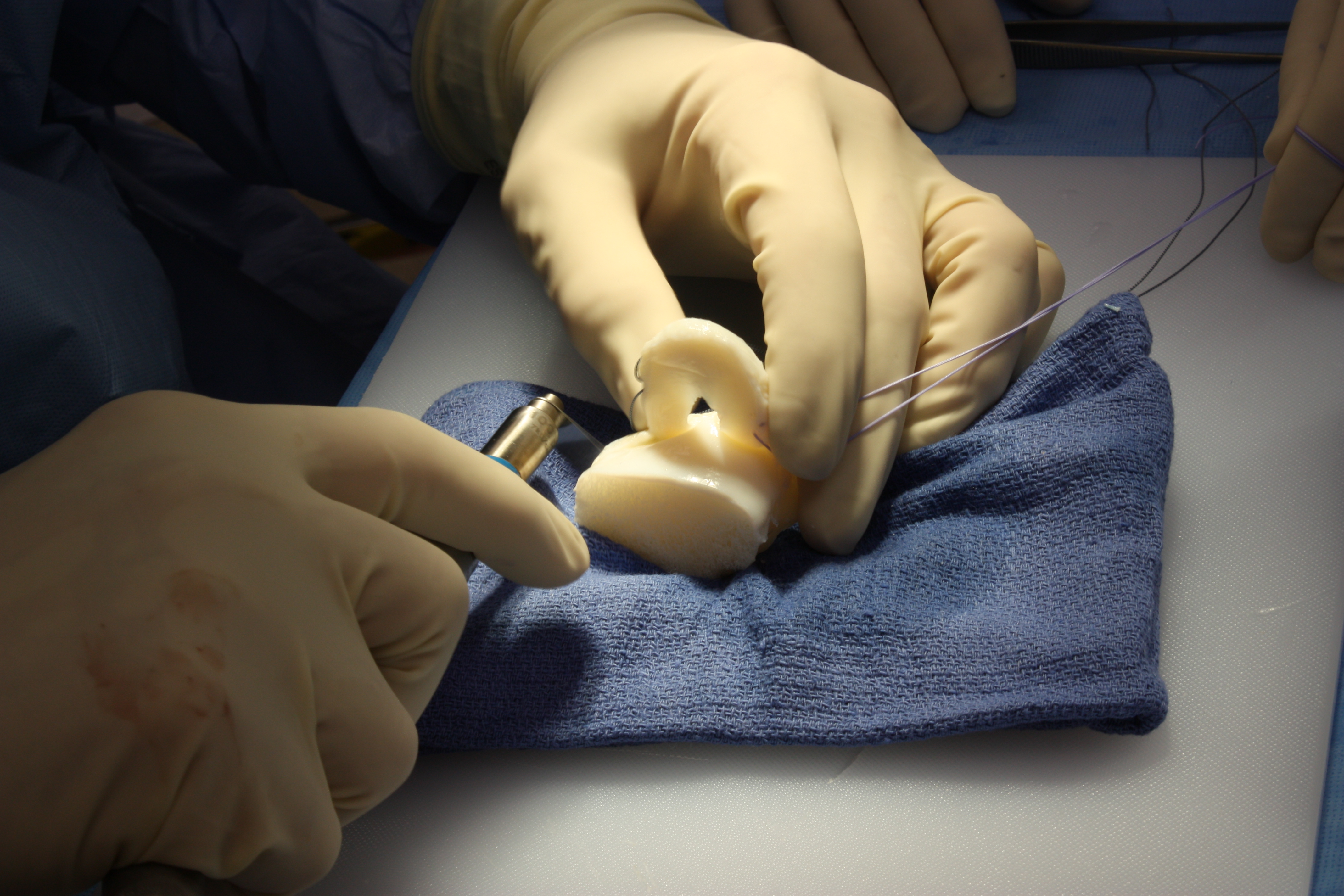
Meniscus Allograft Transplantation (MAT) is a surgical procedure that replaces a damaged or missing meniscus with donor tissue from a cadaver (allograft). When a meniscus is torn beyond repair or has been previously removed, the knee loses its natural shock absorption and force distribution, leading to pain, instability, and accelerated arthritis.
MAT can restore knee function, reduce pain, and potentially delay or prevent the need for total knee replacement. The procedure is typically performed arthroscopically through small incisions, using the three-tunnel technique to secure the donor meniscus to the tibia and surrounding joint capsule.
Recent Research: Studies have shown that meniscus allograft transplantation in conjunction with biologic knee restoration can successfully delay arthroplasty even in patients over 50 years old with moderate to severe arthritis—challenging previous contraindications.
Our Mission
The Meniscus Transplant Study Group (MTSG) advances the science and clinical practice of meniscus transplantation through collaborative research, education, and knowledge sharing among leading orthopaedic surgeons, veterinary surgeons, and scientists worldwide.
Research Excellence
Promoting rigorous scientific investigation into meniscus biology, transplantation techniques, and long-term outcomes.
Education & Training
Facilitating knowledge transfer from basic science research to clinical practice through meetings, presentations, and surgical technique sharing.
Global Collaboration
Connecting international experts to share findings, develop best practices, and improve patient outcomes worldwide.
History
The Meniscus Transplant Study Group (MTSG) was founded in 1986 by a pioneering group of orthopaedic surgeons, veterinary surgeons, and scientists who recognized the need for systematic study of meniscus cartilage transplantation.
Dr. Kevin R. Stone, founder of Stone Research Foundation, was a founding member of the MTSG. Stone Research Foundation has been a driving force behind the group—hosting, facilitating, and funding the annual meeting held in conjunction with the American Academy of Orthopaedic Surgeons (AAOS).
Since its inception, the MTSG has expanded internationally and now includes the European Meniscal Transplantation Group (EMTG). Together, these groups have helped establish meniscus transplantation as a viable treatment option, with over 4,000 human meniscus allografts transplanted and documented outcomes demonstrating significant clinical benefit.
Attend
MTSG 2026 — Porto, Portugal
Kevin R. Stone, MD and the Stone Research Foundation invite you to attend the 2026 Meniscus Transplantation Study Group Meeting, in-person or virtually, at the International Cartilage Regeneration & Joint Preservation Society (ICRS) Summit. Hotel Pestana Douro Riverside, Porto, Portugal.
Thursday, October 8th, 2026 · 11:00am–12:30pm WEST (GMT+1)
Call for Abstracts Is Now Open
We encourage researchers, clinicians, and scientists working in meniscus biology, transplantation techniques, rehabilitation protocols, and outcomes research to submit abstracts for presentation at MTSG 2026 in Porto, Portugal.
Basic science and translational research
Clinical outcomes and case series
Surgical technique innovations
Rehabilitation and recovery protocols
Please upload your abstract below, or email researchteam@stoneresearch.org to submit. Submissions close on September 7th, 2026.
Past Meetings
Click below to access agendas & notes from past meetings.
Resources
Surgical Technique Training
Access comprehensive surgical technique videos for meniscus transplantation, including the three-tunnel technique for medial and lateral meniscus allograft transplantation.
View Technique VideosRehabilitation Program
Evidence-based rehabilitation protocols for meniscus allograft transplantation, developed through decades of clinical experience and outcomes research. Comprehensive rehab protocol PDF coming soon. Contact us for current rehabilitation guidelines and recommendations.
Frequently Asked Questions
Common questions about meniscus transplantation and candidacy.
Stay Connected
Sign up for our newsletter to receive updates on upcoming MTSG meetings, research findings, and educational opportunities. For inquiries about MTSG membership, meeting information, or research collaboration, contact our research team.